
The Mother of All HIV Challenges
Jon Cohen*
Photos by Malcolm Linton
Several studies have shown that cheap, simple treatments can reduce mother-to-child transmission. Applying these advances is another matter
Rachel I. begins to cry, her gaunt frame shaking as she tries to contain her grief. Rachel, 31, is sitting in a social worker's office at a clinic in Abidjan, Côte d'Ivoire, recalling how her life has been torn apart by AIDS.
A few years ago, Rachel, who asked that her last name not be used, lost her first child, a 20-month-old boy. She soon became pregnant again and felt sick herself, so, at her husband's insistence, she finally went to see a doctor. The visit stunned her: She was infected with HIV. When she told her husband, who she believes infected her, he exploded with rage. Fearing for her safety, Rachel moved in with her mother.

Pediatric prospects. A study of nevirapine at this makeshift clinic in Kampala, Uganda, may have found the most practical means yet to curb the staggering rates of mother-to-child transmission in Africa, which accounts for about 90% of global totals (below).
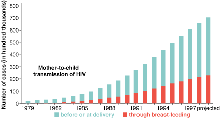
SOURCE: UNAIDS
Through her doctor, Rachel learned of an experimental treatment that might help protect her second baby. Researchers in Europe and the United States had discovered that giving the anti-HIV drug AZT to infected women during pregnancy sharply reduces the chance that the virus will be transmitted to her child. A French-sponsored trial called DITRAME in Côte d'Ivoire and Burkina Faso, headed by François Dabis and Phillippe Van de Perre, was testing whether a simpler--and cheaper--version of the therapy would work in Africa, where between 25% and 35% of babies born to HIV-infected women become infected themselves. Rachel enrolled in the trial and soon heard the first piece of good news she had received in a long time: Her second child, a girl, had been born uninfected.
But tragedy quickly struck again. Like the vast majority of women in Côte d'Ivoire, Rachel breast-fed her daughter. Six months later, she learned that she, too, had become infected, presumably through breast milk. "I haven't been well informed," says Rachel. With help from France's Fund for International Solidarity, Rachel began to treat her baby with the anti-HIV drugs ddI, d4T, and 3TC. But it was too late, says Rachel. Her daughter died at 27 months of age.
Rachel's story epitomizes the dilemma throughout sub-Saharan Africa, where nearly 90% of the half-million babies infected by their mothers each year are born. AIDS researchers are finding cheaper and simpler ways to slow the spread of HIV from mother to child, and more pregnant women, even in the poorest countries, have access to anti-HIV drugs and formula--thanks to the largesse of donors, discounts from industry, new trade laws, and the tenacity of individual clinicians (see profile on p. 2163). But even these advances are barely making a dent in the grim statistics, because just as researchers offer ways to clear one enormous hurdle--drug availability--they run smack into other ones, ranging from social stigmas that discourage testing to disinterest on the part of cash-strapped health authorities to a deeply ingrained culture of breast-feeding--often supported by government policy for otherwise sound health reasons.
"With mother-to-child transmission, many scientific questions have been answered," says DITRAME trial researcher Phillipe Msellati, sitting in an Abidjan café one evening this March. "But now we have to implement things, and the question is, 'How do you do it in reality?' "
Status quo
On Old Mulago Hill in Kampala, Uganda, prehistoric-looking marabou storks stroll on the lawn behind a mustard-colored shack and a canvas tent that helped change AIDS research history.
This shack and tent served as the main clinic and waiting room for a study that involved more than 600 pregnant, HIV-infected women and was run jointly by researchers who work across the street at Makerere University and their collaborators from Johns Hopkins University in Baltimore, Maryland. Half of the women received AZT throughout labor and delivery, and their infants received two doses of the drug each day for the first week of life. In the other group, women in labor swallowed one pill of nevirapine, an anti-HIV drug that the body processes more slowly, and the newborns received one dose of the same medication during the first 3 days after birth. Nearly every woman breast-fed.
In July 1999, an independent group of experts monitoring the trial abruptly ended it because of a startling difference between the babies in the two groups. When they were between 14 and 16 weeks old, 25.1% of the infants in the AZT group had become infected, while only 13.1% in the nevirapine arm were HIV positive. "It blew us all away," says Laura Guay, a Johns Hopkins pediatrician who has lived in Kampala off and on since 1988 and helped run the study.
Guay has since been blown away by a less encouraging statistic: Not a single African country yet offers this $4 regimen of nevirapine to HIV-infected pregnant women, nearly 4 years after the drug came on the U.S. market. And only Uganda, Kenya, and South Africa have licensed it for sale. "It makes no sense to me," says Guay, sitting in her office, located in a new building (built with Johns Hopkins funds) up the hill from the clinic. "In my talks with several government representatives from countries around here, they raise a lot of questions: 'We don't know about long-term toxicities, we don't know about drug resistance, so we're not going to do anything.' It's incredible." By contrast, she says, when 076 came out, wealthy countries worldwide implemented it within weeks.
Guay's shorthand mention of "076" refers to a study that provided the first convincing data indicating that anti-HIV drugs could reduce mother-to-child transmission of HIV. A drug regimen tested in the study--which was sponsored by the U.S. National Institutes of Health, as was the nevirapine study--cut the transmission rate by nearly 70%. But it had next to no relevance to poor countries, as the treatment cost about $800 and required an intravenous drip of AZT during labor. Further complicating matters, most women took the drug for 11 weeks before birth and none breast-fed. Poor African women, in contrast, often don't seek medical help until they go into labor, and most breast-feed.
In the 5 years between the headlines that celebrated the 076 results and those from the nevirapine study, several cheaper, simpler versions of 076 had proven themselves. Trials in Thailand, Uganda, South Africa, Tanzania, and Côte d'Ivoire, including the DITRAME study that Rachel I. joined, all showed that a short course of AZT or a combination of AZT and 3TC in the last month of pregnancy could lower the risk of transmission by up to 50%. Nevirapine promises similar or better results--with a much cheaper and simpler regimen.
The breast-feeding dilemma
A big question mark hangs over all of these studies: the risk of long-term breast-feeding. The PETRA trial--the largest mother-to-child transmission study to date, with 1792 enrolled--has reported data from only 6 weeks after birth; many African mothers breast-feed for the first few years of life. When continued breast-feeding is factored in, "the data will not be all that rosy," predicts Fred Mhalu, a leading AIDS researcher at Tanzania's Muhimbili University, one of the PETRA sites.
There's little question that breast-feeding greatly increases the risk of transmission. A 6-year study, conducted in Nairobi and published on 1 March in The Journal of the American Medical Association, compared infected mothers who used infant formula--provided by the study--to those who breast-fed (Science, 11 February, p. 942). Of the babies born uninfected, the study showed that formula-fed children had 16% fewer HIV infections at 2 years of age than the ones who exclusively breast-fed (for 17 months, on average). "We showed that in an urban setting with potable water, poor HIV-infected women with very limited education can use formula, and their children clearly have a much better outcome," says Joan Kreiss of the University of Washington, Seattle, who conducted the study with the University of Nairobi's Ruth Nduati and co-workers.
The simple implication is that clinicians should discourage HIV-positive mothers from breast-feeding. But, as the University of Nairobi's Dorothy Mbori-Ngacha acknowledges, what sounds simple is, in reality, "a very challenging intervention" in an African setting. Many governments and international aid organizations have long promoted breast-feeding. Not only does formula cost more than many people earn, but many have no access to clean water, increasing the risk that formula itself can cause life-threatening diarrheal disease. The Nairobi study indicated that formula can be used safely in some situations, but "safe water is a big deal," says Mbori-Ngacha. "Without it, formula becomes something you don't even want to discuss."
Even if clean water is available, there are fundamental barriers to bottle-feeding. "If you don't breast-feed your baby, you're announcing that you're HIV positive," says the University of Manitoba's Frank Plummer, who has lived in Nairobi for the past 16 years. "If you're on a bus and your baby starts crying, people will start yelling at you to breast-feed the baby." Indeed, given nevirapine's potential for cutting transmission rates, "to us, the major risk factor now is the stigma of not breast-feeding," says Hopkins's Guay.
Social barriers
In the end, the social stigma of being HIV positive presents the most intractable problem health workers face in trying to prevent infected African women from transmitting the virus to their babies. Many women, fearing the angry reaction Rachel's husband displayed, don't even tell their partners their HIV status--even though many are infected because of their partner's infidelity. Such fears discourage many women from even being tested. "It's one of the areas we've neglected till now: sociobehavioral research," says Thierry Roels, an official at Projet RETRO-CI. "We assumed if we found something, people would take it."
The RETRO-CI study indicates that such an assumption is not well founded. In February 1998, researchers at RETRO-CI offered pregnant women in Abidjan free HIV tests and counseling. They offered those who tested positive free AZT at 36 weeks of gestation through delivery. More than 9600 pregnant women visited the clinic during this study, 72% of whom agreed to be tested. Thirteen percent tested positive. But of those, only 46% returned to learn the test results. And at 36 weeks of gestation, the researchers could find only 70% of the infected group. Most of these 117 women took AZT, but they represented a mere 12.6% of those who tested positive in the study. "One of the problems is [that] between screening and enrollment in the study, there's a long period," explains Sibailly Toussaint, who heads the mother-child division of RETRO-CI.
With this in mind, the RETRO-CI team developed a rapid test that determines HIV status in hours rather than weeks. This enabled the researchers to test women and enroll them for treatment on the same day. Of the nearly 4000 pregnant women offered the test, 68% took it and 10.9% were positive. More than 75% of the women stuck around to learn their results--a big improvement. But half never showed up for treatment. In the end, only 37 of 294 infected women--again, 12.6%--took AZT.

C'est arrive! Philippa Musoke (right) and Laura Guay inventory a long-awaited nevirapine delivery in Kampala.
Toussaint remains optimistic, though, that a simple regimen of one dose of nevirapine to mother and child might vastly improve these numbers. "Imagine using the rapid test and we give them the pill and tell them to take it when they go into labor," says Toussaint. "We think we could reduce transmission significantly."
D-Day
Toussaint's optimism may soon be put to the test. On 20 March, Guay and Makerere University's Philippa Musoke, another principal researcher in the nevirapine study, excitedly watched a small truck pull into their parking lot on Old Mulago Hill. Inside was the first delivery of nevirapine sent to Africa as part of a project that will offer infected, pregnant women the drug free of charge, without even enrolling them in a study.
Similar nevirapine deliveries--part of an $800,000 effort funded by the Pediatric AIDS Foundation--soon will arrive in Rwanda, Kenya, South Africa, and Cameroon. Pharmaceutical companies have cut prices. Special projects launched by the U.S. and French governments will attempt to reach and treat pregnant women throughout Africa.
Clinician Eric Mercier oversees an ambitious $4 million project funded by the United Nations Children's Fund, with AZT donated by Glaxo Wellcome, that also delivers drugs and formula to eight African countries. Mercier says the world must provide treatments as quickly as possible or pregnant women will take worthless medications. "There are plenty of fake drugs around the world, and women don't want to infect their children," says Mercier. "They'll take anything." In the same breath, Mercier urges patience, too. "We're in a world where people want to see immediate change and results. It's important to start now: People will use it, [and] others will see it and come into it. But it takes time."
* Jon Cohen was accompanied by photographer Malcolm Linton. For a gallery of additional photos and the stories behind them, see
www.sciencemag.org/feature/data/aids_africa/gallery.shl.
Volume 288,
Number 5474,
Issue of 23 Jun 2000,
pp. 2160-2163.
Copyright © 2000 by The American Association for the Advancement of Science.
|