
Is AIDS in Africa a Distinct Disease?
Jon Cohen*
Photos by Malcolm Linton
Opportunistic infections, transmission patterns, and viral subtypes differ, but there are more similarities than differences in HIV's behavior in Africa
Researchers and policy-makers around the world groaned when they learned of the fiery letter South African President Thabo Mbeki sent world leaders on 3 April, defending his decision to seek advice from "dissidents" who question whether HIV causes AIDS. Most dismissed Mbeki's infatuation with contrarian thought as dangerously misguided (see p. 2168). But his letter did highlight a fact that few AIDS researchers would challenge: "It is obvious that whatever lessons we have to and may draw from the West about the grave issue of HIV/AIDS, a simple superimposition of Western experience on African reality would be absurd and illogical," wrote Mbeki.
Although AIDS researchers have solid data that suggest anti-HIV drugs work as well in Africa as anywhere else--removing a cornerstone of Mbeki's argument--many share the South African president's conviction that the African AIDS epidemic has unique features. As Mbeki noted, homosexual spread of HIV accounts for the majority of AIDS cases in the United States and Europe, while Africa has a primarily heterosexual epidemic. HIV also has spread more quickly in Africa, where different strains of the virus predominate. And AIDS-related diseases--and possibly disease progression itself--differ in Africa, too.
Yet 2 decades into the epidemic, AIDS researchers have only a shaky handle on the fundamental question: What accounts for these differences?

Purple puzzle. This man in Gulu, Uganda, has Kaposi's sarcoma, a relatively common disease in Africa that's largely restricted to HIV-infected gay men elsewhere.
The answers have potentially important implications. "We'd like to know whether we could develop appropriate strategies for AIDS patients," explains Gaston Djomand, head of the clinical section at Projet RETRO-CI in Abidjan, Côte d'Ivoire. "It makes a difference to know whether patients die 2 years after diagnosis of AIDS or 5 years. You can develop strategies to prolong healthy lives." It also makes a difference to know whether the HIV strains circulating in Africa or the immune systems of people living there have special characteristics, two other topics that have attracted much attention--and debate.
Location, location, location
The most obvious difference is clinical, and you don't need a medical degree to see it. Lacor Hospital in Gulu, Uganda, has a ward with a fenced-off courtyard, where many patients spend their days sitting with their families on bamboo mats, escaping the heat under blooming jacaranda and tulip trees. The courtyard has a graceful and peaceful feel, like a tuberculosis sanitarium from the past century. In fact, it is a TB sanitarium, but it is also largely an AIDS ward: Roughly 50% of the 100 patients, who stay for 2 months of treatment, are also infected with HIV.
Tuberculosis kills more HIV-infected people in Africa than any other AIDS-related disease. A study by the RETRO-CI research team, for example, found TB in 40% of HIV-infected people upon autopsy. In contrast, TB remains relatively rare in AIDS patients in the United States and Europe. Eleizer Masliah, a neurologist and pathologist at the University of California, San Diego (UCSD), recently found no TB at all in 390 autopsies of people who died from AIDS. "It's kind of surprising here, next to the [Mexican] border, where you'd expect to see more cases," says Masliah. Similarly, Kaposi's sarcoma, a cancer that causes purple skin blotching, commonly afflicts HIV-uninfected and -infected people in Africa, while in industrialized countries it's largely restricted to HIV-infected, gay men.
Pneumocystis carinii pneumonia (PCP) shows the opposite pattern. Although malnourished African children have long suffered from PCP and many Africans have antibodies to the protozoa--indicating that it is common there--the RETRO-CI researchers only found P. carinii in 8% of the HIV-infected people autopsied. Similar results came from autopsy studies in Uganda and the former Zaire. Yet during the 1980s, PCP infected more than 80% of AIDS patients in developed countries at some time during the course of the disease, and the UCSD team found the protozoa in 30% to 40% of patients they autopsied. (Thanks to effective treatments for PCP and HIV, PCP rates in the late 1990s declined dramatically in developed countries; the UCSD study found the protozoa in only 7.6% of the 1998 autopsies.)
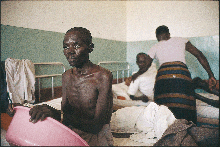
Common culprit. TB patient in Uganda's Lacor Hospital. TB is the most common cause of AIDS-related deaths in Africa.
Although the contrasts may be starker than expected, researchers say the overall pattern is not surprising. "To some extent, what you see in HIV-positive people reflects what you see in the general population," says James Whitworth of the U.K.'s Medical Research Council, which funds the AIDS program he co-directs with Anatoli Kamani at the Uganda Virus Research Institute in Entebbe. Tuberculosis, he notes, is much more common in Africa, and although he sees PCP autopsy data as "a big conundrum," he suspects that many clinicians might miss it because it's relatively difficult to diagnose in Africa.
Whitworth is equally skeptical of claims that in Africa the disease typically progresses more rapidly from infection to AIDS to death. In the United States and Europe before anti-HIV drugs existed, gay men on average developed AIDS in 10 years and died in 12. In Africa, however, studies have come up with different results. One study, by the University of Nairobi's Omu Anzala and co-workers, found that Nairobi sex workers on average developed AIDS 4.4 years after infection, but the same researchers found that the disease progressed much more slowly in infected, pregnant Nairobi women. The difference, they surmised, may have been a result of high rates of sexually transmitted diseases (STDs) among the sex workers.
Whitworth, Dilys Morgan, Martin Okongo, and other members of his team have found rates of disease progression in the general population in Masaka, Uganda, similar to those seen in developed countries. Eight years into the study, about 40% of the people had developed AIDS, with death occurring 9 to 10 months later. Whitworth concludes that AIDS in the Masaka district looks like AIDS anywhere else. "There are lots of nasty diseases around here," says Whitworth. "But with decent medical care, HIV-infected people in Africa can live as long as people in Europe and the West did before the era of antiretrovirals."
Ease of infection
Perhaps the sharpest disparity of all is the relative ease with which HIV seems to infect Africans. In studies conducted in the United States by researchers working with the U.S. National Institutes of Health to prepare for vaccine trials, high-risk populations such as gay men have had new infection rates of 2% per year. In some African populations, new infection rates are six times higher.
A combination of higher rates of untreated STDs, limited prevention campaigns, and lack of access to health care in general may account for much of the difference. But researchers are looking into two other possible factors: whether African immune systems are more vulnerable to HIV, and whether strains of the virus circulating in Africa may be more infectious than those circulating in the United States and Europe.
In an unusual study, the University of Milan's Mario Clerici, Lacor Hospital's Matthew Lukwiya (see profile on p. 2159), and their co-workers compared immune cells from two groups of people who were not infected with HIV: Ugandans and Italians living in Gulu versus Ugandans and Italians living in Milan. They found stark differences by location, but not by genetic background.
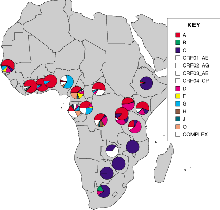
C sickness. Subtype C has taken over as the main strain of HIV in southern Africa.
SOURCE: VADIM ZALUNIN/LOS ALAMOS NATIONAL LABORATORY
The researchers reported in the December 1998 issue of the journal AIDS that the immune systems of people living in Africa appear to be more highly "activated," presumably because they must constantly fend off a much broader range of diseases. And a higher level of activation should mean more CD4 cells--HIV's main target--circulating in the blood. "You get more targets, you keep the virus happy," says Clerici. Whitworth's lab has found some evidence to support this idea, but he remains skeptical. "There are loads of hypotheses, and which ones hold water, I don't know," says Whitworth.
Theories about the impact of viral differences on ease of infection are focusing on a strain of HIV-1 known as subtype C--one of 11 subtypes, labeled A to K, of the most common group of HIV viruses. Subtype B predominates in the United States and Europe, rarely showing up in Africa, other than in South African homosexuals. East Africa has mostly subtypes A and D, while west Africa has predominately A and a combination A/G virus. (HIV-2, a distinctly different type of the virus, is also endemic to west Africa, but it has spread to other parts of the continent and the world. With Harvard University's Max Essex and Phyllis Kanki, Souleymane M'boup of Cheikh Anta Diop University in Dakar, Senegal, has helped establish that HIV-2 causes AIDS much more slowly than HIV-1 does.) In southern Africa, which had little HIV-1 until the 1990s, subtype C accounts for most of the infections. "The fact that C is circulating so rapidly is fascinating, and I tend to think it's different," says Bette Korber, who oversees the HIV database at New Mexico's Los Alamos National Laboratory.
One difference, seen in studies of isolates from Malawi and Ethiopia, is in the cell surface receptors that HIV docks onto. HIV initially attaches to both a CD4 receptor and a coreceptor called CCR5 to establish an infection. Typically, as a person's immune system wears down, HIV begins favoring another coreceptor, CXCR4, over CCR5. But subtype C rarely makes the switch. This means that at any given time, a person infected with subtype C will likely have more copies of the virus that dock with CCR5--the variant most capable of establishing an initial infection.
Essex also believes that subtype C may transmit more efficiently through heterosexual sex. In the January Journal of Infectious Diseases, Essex and co-authors describe a chemical messenger secreted by immune cells that boosts HIV replication, particularly that of subtype C. Because venereal diseases increase secretion of this messenger, the researchers write that "it is tempting to speculate" that these conditions may explain the explosive spread of subtype C.
Other researchers see these speculations as just that. Saladin Osmanov, who tracks subtypes for the Joint United Nations Programme on HIV/AIDS, suspects that subtype C's current front-runner slot may simply be part of the ebb and flow of the epidemic. "Viruses tend to shift and disappear and come back," says Osmanov. "I don't like simple explanations." Virologist Martine Peeters of the Institute of Research for Development in Montpellier, France, agrees. "There are almost no subtype C data," says Peeters, who has worked extensively in Gabon, Cameroon, and Senegal. "It's too early to conclude anything about any subtypes."
HIV and AIDS do have different characteristics in Africa, but most researchers, ultimately, never lose sight of the main similarity: HIV, everywhere it goes, destroys immune systems, cuts lives short, and devastates communities. In Masaka, Uganda, says Whitworth, the risk of death increases by 11 times in people who test positive for HIV. Yet Whitworth says he also appreciates the Thabo Mbekis of the world: "It makes us think about assumptions and be quite sharp in our arguments."
* Jon Cohen was accompanied by photographer Malcolm Linton. For a gallery of additional photos and the stories behind them, see www.sciencemag.org/feature/data/aids_africa/gallery.shl.
Volume 288,
Number 5474,
Issue of 23 Jun 2000,
pp. 2153-2155.
Copyright © 2000 by The American Association for the Advancement of Science.
|